Kidney Topics
Living Kidney Donor Evaluation
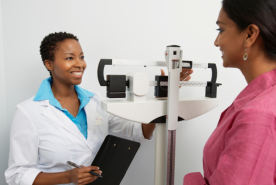
The kidney donor process starts by contacting a transplant center to get evaluated. You’ll meet with the living donor team and have other testing done...
Organ and tissue transplantation and donation,
Living donor evaluation