Osteoporosis: What You Need to Know
Brandon Viehmann PT, DPT

Osteoporosis or bone thinning is a prevalent systemic disease that results from a variety of risk factors that may occur throughout your life. Osteoporosis is commonly referred to as a “silent disease” because signs and symptoms may not be obvious. It is common for individuals who have not been adequately screened to be diagnosed with osteoporosis when they sustain a broken bone (a low level impact fracture). Fracture sites are common in the hip, mid to low-back, rib cage, distal forearm and pelvis.
It has been estimated that there are currently over 50 million individuals in the United States that are at risk for developing osteoporosis. Risk factors for the disease include age, fluctuations in hormone levels in the body, poor diet, low activity levels, genetic predisposition, mal-absorption syndromes in the digestive tract, and transplantation. The majority of cases of osteoporosis involve post-menopausal Caucasian women due to the sudden decrease in estrogen levels in the body, but men and individuals from other races are not immune to bone thinning. The Hispanic population has the fastest growing rates of diagnosed cases of osteoporosis worldwide.
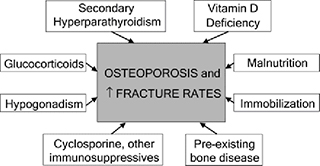 For transplant recipients, osteoporosis is usually caused by a variety of factors related to the end stage chronic disease: immunosuppressive medications, corticosteroids, and decreased levels of physical activity. The rate of bone loss is greatest within the first 6 to 12 months post-transplant due to the stress of surgery, high immunosuppressive and corticosteroid medication dosage, and the adverse effects of organ failure. The risk of osteoporosis increases again years after transplantation, with the incidence as high as 40% depending upon the type of organ transplanted. Lung and liver transplant recipients have the highest incidence of osteoporosis-related fractures.
For transplant recipients, osteoporosis is usually caused by a variety of factors related to the end stage chronic disease: immunosuppressive medications, corticosteroids, and decreased levels of physical activity. The rate of bone loss is greatest within the first 6 to 12 months post-transplant due to the stress of surgery, high immunosuppressive and corticosteroid medication dosage, and the adverse effects of organ failure. The risk of osteoporosis increases again years after transplantation, with the incidence as high as 40% depending upon the type of organ transplanted. Lung and liver transplant recipients have the highest incidence of osteoporosis-related fractures.
It has been recommended by the United States Preventative Services Task Force that all women over the age of 60 be screened for bone thinning. If a female has a personal history or maternal history of fractures, screening should begin at age 50. Most transplant centers require pre-transplant screening and continued screening post-transplant to monitor and aggressively treat any signs of bone disease.
Scanning for at risk individuals is important to reduce the risk of bone fractures. Screening is a simple, painless and non-invasive process that is accomplished by using a DEXA (Dual-energy X-ray absorptiometry) machine. In addition to a DEXA scan, balance, musculoskeletal and pulmonary function testing should be taken into consideration. A DEXA scan typically measures an individual’s bone mineral density (BMD) at the lower back, the neck of the femur (thigh bone), or the distal forearm (wrist).
This BMD score is then compared to the peak bone mass of a healthy individual which typically occurs at 30 years of age. A normal score is represented as -1.0. Osteopenia or mild bone thinning is demonstrated with a score ranging from -1.0 to -2.5. A score within this range places the individual at risk for developing osteoporosis. Any score of -2.5 or greater is indicative of osteoporosis at the measured location.
If osteopenia or osteoporosis is diagnosed, you can control the progression of the disease or in some cases even reverse bone thinning via a combination of exercise, diet and dietary supplements, and medication use. If you are not having a routine DEXA scan, you should talk to your transplant coordinator or doctor about making a BMD screening part of your regular health and wellness check-ups.
A comprehensive exercise program is an important part of preventing and treating osteoporosis. Poor posture can lead to musculoskeletal problems and maintaining good posture during exercises can decrease your risk of further injuries. Strengthening the back extensor muscles has been shown to decrease the frequency of back pain and compression fractures in individuals with osteoporosis. Additionally, cardiovascular endurance training combined with resistance training (strengthening exercises) has been shown to increase bone density and strengthen the muscle tendons attached to the bone. Incorporating balance or coordination training along with flexibility exercises is essential to a comprehensive exercise regimen.
As there are precautions to take before beginning an exercise routine, a consultation with the appropriate medical professional is essential. Qualified and licensed physical therapists are medical professionals that can assist you in establishing a safe and progressive exercise program to help manage your bone health and to treat osteoporosis and its complications. A physical therapist is specially trained in musculoskeletal diseases. As such, physical therapists can provide you with an individualized plan to help prevent and slow the disease process.
