Key points: About Dialysis for Kidney Failure
Contents
- Dialysis and kidney transplant are both treatments for kidney failure
- You don't have to feel "locked in" to any one type of dialysis. There are advantages and disadvantages for each. If you wish to change your current treatment choice, speak to your healthcare professional.
- Even if you are already receiving dialysis, it may be possible to have a kidney transplant
- When you are on dialysis, it is important for you to:
- Come to every dialysis treatment and stay for the entire treatment.
- Learn what you can do to keep as much kidney function as you have left - and do it!
- Do your part to help manage the complications of kidney disease and kidney failure
- Heart and blood vessel problems
- Anemia (low red blood cell count)
- Bone problems
- High blood pressure
- Poor nutritional health (i.e. happens when you are not getting enough important nutrients and energy for your body to function and stay healthy)
- Manage any other health problems you may have that could cause your condition to get worse, such as diabetes
What is Kidney Failure?
Kidney failure does not happen overnight. In the early stages of kidney disease, there are few, if any, symptoms. Symptoms usually show up late in the process. Kidney failure is the end result of a typically gradual loss of kidney function. The most common causes of kidney failure are diabetes and high blood pressure. Kidney failure happens when:
- 85-90% of kidney function is gone
- GFR falls below 15
- Kidneys don't work well enough to keep you alive
As your kidneys failed, the level of creatinine in your blood rose. The amount of creatinine in your blood is a factor used in calculating your GFR (glomerular filtration rate, a measure of kidney function). As creatinine goes up, GFR goes down. In kidney failure some of you may have nausea, vomiting, a loss of appetite, weakness, increasing tiredness, itching, muscle cramps (especially in the legs) and anemia (a low blood count). With treatment for kidney failure, these symptoms will improve and you will begin to feel much better.
There is no cure for kidney failure, but with treatment it is possible to live a long, fulfilling life. Having kidney failure is not a death sentence. People with kidney failure live active lives and continue to do the things they love.
Treatments for Kidney Failure
The two treatments for kidney failure are kidney transplantation and dialysis. Two different types of dialysis can be done - hemodialysis and peritoneal dialysis.
- Kidney Transplantation. This is an operation that places a healthy kidney into your body. The kidney can come from someone who has died or from a living donor. A new kidney will usually function immediately. You will need special medicines to prevent your body from rejecting the new kidney. If rejection happens, dialysis is needed and you can consider a second transplant. A kidney transplant is a treatment, not a cure. Kidney transplant recipients still have chronic kidney disease, and you may still need some of the other medicines they took before the transplant.
Even if you are already receiving dialysis, it may be possible to have a kidney transplant. If you are interested in learning more about kidney transplant and finding out if you are a candidate for a transplant, ask your healthcare professional and contact the National Kidney Foundation (www.nkfcares.org or 1-800-622-9010). You can also learn more transplantation, by searching the A-to-Z Guide for "Am I a Candidate for Kidney Transplantation". - Hemodialysis (HD). Hemodialysis is a treatment that removes wastes and extra fluid from your blood. It can be done at home ("home hemodialysis") or in a dialysis center. During hemodialysis, your blood is pumped through soft tubes to a dialysis machine where it goes through a special filter called a dialyzer (also called an artificial kidney). As your blood is filtered, it is returned to your blood stream. Only a small amount of blood is out of your body at any time. In-center treatment time is 3-5 hours, 3 times a week. People who do home hemodialysis have more flexibility about how often it can be done. If done daily, treatment time would be 1½ to 2 hours. You will need an access into the bloodstream for placing needles needed for hemodialysis. Types of access include:
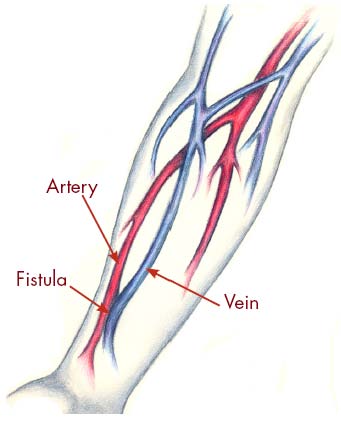 Fistula. A fistula is the recommended choice for an access. You will need a minor operation to create a fistula. It is made by joining an artery to a nearby vein under your skin to make a bigger blood vessel. This type of access is preferred because it has fewer problems and lasts longer. However, some people may not be able to have a fistula because of their physical condition. Sometimes, it may be possible to switch to a fistula from another type of access. If you do not have a fistula, ask your dialysis care team if a switch would be possible.
Fistula. A fistula is the recommended choice for an access. You will need a minor operation to create a fistula. It is made by joining an artery to a nearby vein under your skin to make a bigger blood vessel. This type of access is preferred because it has fewer problems and lasts longer. However, some people may not be able to have a fistula because of their physical condition. Sometimes, it may be possible to switch to a fistula from another type of access. If you do not have a fistula, ask your dialysis care team if a switch would be possible.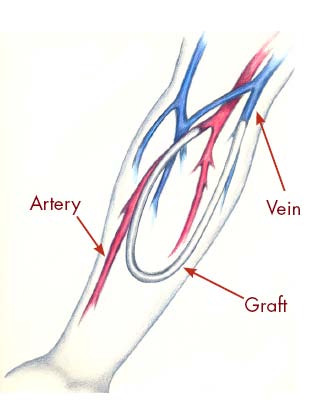 Graft. If your blood vessels are not suitable for a fistula, a graft may be used. This involves joining an artery and a nearby vein with a small, soft tube made of synthetic material. The graft is entirely beneath your skin. You will need a minor operation to create a graft.
Graft. If your blood vessels are not suitable for a fistula, a graft may be used. This involves joining an artery and a nearby vein with a small, soft tube made of synthetic material. The graft is entirely beneath your skin. You will need a minor operation to create a graft.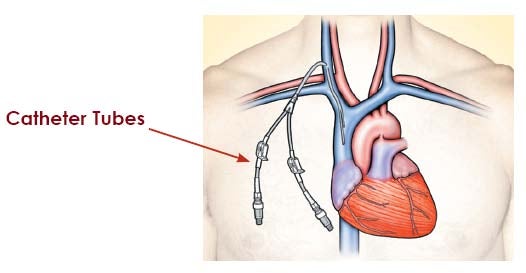 Catheter. The third type of access, called a catheter, is inserted into a large vein in your neck or chest. The ends of the tubes sit on your skin outside your body. This type of access is generally used when you need dialysis for a short period of time. Catheters are used as a permanent access when a fistula or a graft cannot be placed.
Catheter. The third type of access, called a catheter, is inserted into a large vein in your neck or chest. The ends of the tubes sit on your skin outside your body. This type of access is generally used when you need dialysis for a short period of time. Catheters are used as a permanent access when a fistula or a graft cannot be placed.
- Peritoneal Dialysis (PD). Peritoneal dialysis is a home-based treatment that can be done anywhere (at home, work, or when sleeping). It must be done daily. You will need a minor operation to place a catheter in your abdomen (belly). With peritoneal dialysis, the blood is cleaned inside your body, not outside. The lining of your abdomen (the peritoneum) acts as a natural filter. During treatment a cleansing solution, called dialysate, flows into your abdomen (your belly) through a soft tube called a PD catheter.Wastes and extra fluid pass from your blood into the cleansing solution. After several hours, you drain the used solution from your abdomen and refill with fresh cleansing solution to begin the process again. Removing the used solution and adding fresh solutions takes about a half hour and is called an "exchange."
To learn more about each type of treatment, see "Choosing a Treatment for Kidney Failure" in the A-to-Z Guide.
Choosing Dialysis
There are advantages and disadvantages to each type of dialysis treatment. (If you think one type of dialysis may be better for you than the type you are now on, it may be possible to change.) You don't have to feel "locked in" to any one type of dialysis. You should start by knowing the advantages and disadvantages for each one, and speak to your healthcare professional. The charts below will help you to compare some of the pros and cons of the different types of dialysis.
| Advantages | Disadvantages |
|---|---|
|
|
| Advantages | Disadvantages |
|---|---|
|
|
| Advantages | Disadvantages |
|---|---|
|
|
Self-Management
Good self-management will help you to live a longer, more active life and continue to do the things you love. It will also help you to preserve the remaining kidney function you have left. Even after kidneys fail, you will still have some remaining kidney function left. It is important to keep as much of this as you can. This will help improve your health and enable you to live longer and better. Good self-management starts with:
- Getting enough dialysis
- Caring for your hemodialysis access or peritoneal catheter
- Following the medical plan that was recommended to manage heart and blood vessel problems, high blood pressure, anemia, bone problems, poor nutrition and diabetes if you have it.
- Adopt healthy lifestyle behaviors like not smoking, eating right and getting enough exercise.
Getting Enough Dialysis
It is important that you get enough dialysis. Studies have shown that getting the right amount of dialysis improves your overall health, makes you feel better, keeps you out of the hospital, and enables you to live longer. Your healthcare professional will give you a "dialysis prescription" to make sure you get the right amount of treatment. It depends on:
- How well your kidneys work
- How much fluid weight you gain between treatments
- How much waste you have in your body
- Your body weight
- The type of artifical kidney used your dialysis center (if you are doing in-center hemodialysis)
Your dialysis care team will monitor your treatment with monthly lab tests to measure the amount of dialysis you receive. This is called your "delivered dose of dialysis." The number that tells your delivered dose of dialysis is your Kt/V (pronounced "kay tee over vee"). The goal for your Kt/V number may vary depending on how often you have dialysis and on how much remaining kidney function you have left. For many hemodialysis patients who have three treatments weekly, Kt/V should be at least 1.2 for each treatment. For people receiving peritoneal dialysis, it should not be less than 1.7 per week.
Other methods are sometimes used to measure delivered dose of dialysis. For example, some dialysis centers may use the urea reduction ratio (URR). If this ratio is used to measure your delivered dose of dialysis, your URR should be at least 65 percent for each treatment.
Caring for Your Access
Another part of good self-management is caring for your fistula, graft, or catheter.
To protect and care for your hemodialysis fistula or graft:
- Do not let anyone measure your blood pressure on your access arm. Your other arm should be used instead.
- Do not let anyone take blood from your access arm.
- If the vibration (thrill) or sound (bruit) of your access is absent or seems different, call your dialysis care team at once. This could mean the access is not working well.
- Ask your dialysis care team how to make your needle sticks as comfortable as possible. They can use different sites for the needles during each dialysis. Or, if you have a fistula, a "button hole" technique may be used. This uses the same site for each dialysis, and may be less painful.
- Prevent infection
- Ask your dialysis care team to teach you about preventing infection and keeping your fistula or graft working well.
- Wash your access site every day with an antibacterial soap. Ask your dialysis care team to recommend a good soap to use.
- Wash access site before every dialysis treatment. Your dialysis center has hand washing sinks and antibacterial soap.
- Do not scratch your access. Your fingernails could be a source of infection.
- Your nurse or technician should clean your access site with an antiseptic before putting the needles in. Do not touch your access area after it has been disinfected.
- Your nurse or technician should wear a surgical mask, a face shield and clean gloves when working near your access.
- Avoid coughing or sneezing on your access site during treatment.
- Always wear a clean glove or use a clean gauze pad if you are holding your own access site after the needles are pulled.
- Apply only gentle pressure to stop bleeding after the needles are removed. Press only where the needle was and just below. Never press above where the needle was.
- Call your dialysis care team at once if the area of the access is sore, swollen, red or feels hot. This could be a sign of infection.
To protect and care for your hemodialysis catheter, you should:
- Prevent infection
- Ask your dialysis care team to teach you how to prevent infections and keep HD your catheter working well.
- Be sure your catheter has a clean, dry dressing during and after every dialysis. Make sure your nurse or technician checks your catheter for signs of infection at every visit.
- Make sure you wear a surgical mask when you are being connected to or disconnected from the dialysis machine.
- Make sure your nurse or technician wears a surgical mask, face shield and clean gloves when working near your catheter.
- Ask your nurse or technician to teach you or your family how to change the dressing.Keep extra dressing supplies at home in case you need to replace your dressing.
- Keep extra dressing supplies at home in case you need to replace your dressing.
- Call your dialysis care team right away if your catheter cuff is showing.
To protect and care for your peritoneal catheter, you should:
- Check your PD catheter every day for signs of cracking or pulling
- Do not wear tight clothes and belts around the exit site
- Wash your hands with soap and water for at least two minutes and dry them with a disposable paper towel before handling your PD catheter, and before and after an exchange is made
- Tape the PD catheter down to your skin
- Keep the PD catheter away from scissors or other sharp objects
- Cleanse the PD catheter thoroughly with a wash cloth and soap every day
- Keep a special dressing over the exit site if your dialysis care team tells you to do so
- Do not allow tugging or pulling of your PD catheter
Managing Other Health Problems
Chronic kidney disease can cause other problems throughout your body including:
- Heart and blood vessel problems
- Anemia (low red blood cell count)
- Bone problems
- High blood pressure
- Poor nutritional health
Kidney disease does not happen overnight. You may have been experiencing some of these problems for many years before your kidneys failed. Your healthcare professional will work with you to develop a treatment plan to help you manage these problems and keep them from getting worse. Treatment usually includes diet, exercise, and medications. It is very important that you follow your treatment plan because it can greatly improve your quality of life and how long you live. It can also help to protect the remaining kidney function you have left.
To learn more about the treatments for the problems listed above, see the A-to-Z guide.
Tools to Help
- Track Your Important Dialysis Measurements

- Fluid Diary

- Activity Schedule

- My Wellness Goals

- A "New Normal": Life on Dialysis - The First 90 Days. Helpful advice from people on dialysis.
To Learn More
You can learn more about kidney failure in the A-to-Z guide:

- About Chronic Kidney Disease: A Guide for Patients and Their Families
- GFR
- Choosing a Treatment for Kidney Failure
- Kidney Transplant
- A Guide to Heart Health for Dialysis Patients
- Mineral and Bone Disorder
- Diabetes and Kidney Disease
- Hemodialysis
- Hemodialysis Access: What You Need to Know
- Anemia
- Peritoneal Dialysis: What You Need to Know
- Diet and Nutrition
