About the Initiative
Nearly 2 million adults in Virginia and Metro DC are living with chronic kidney disease (CKD), but more than 1.75 million may not be aware. Fewer than 20% of people with risk factors for CKD (diabetes and/or hypertension) are tested appropriately.
As part of a national NKF Collective Impact strategy, Virginia stakeholders are implementing a roadmap to drive a cultural shift in primary care- toward increasing the early diagnosis and management of CKD, especially in communities disproportionately burdened by CKD.
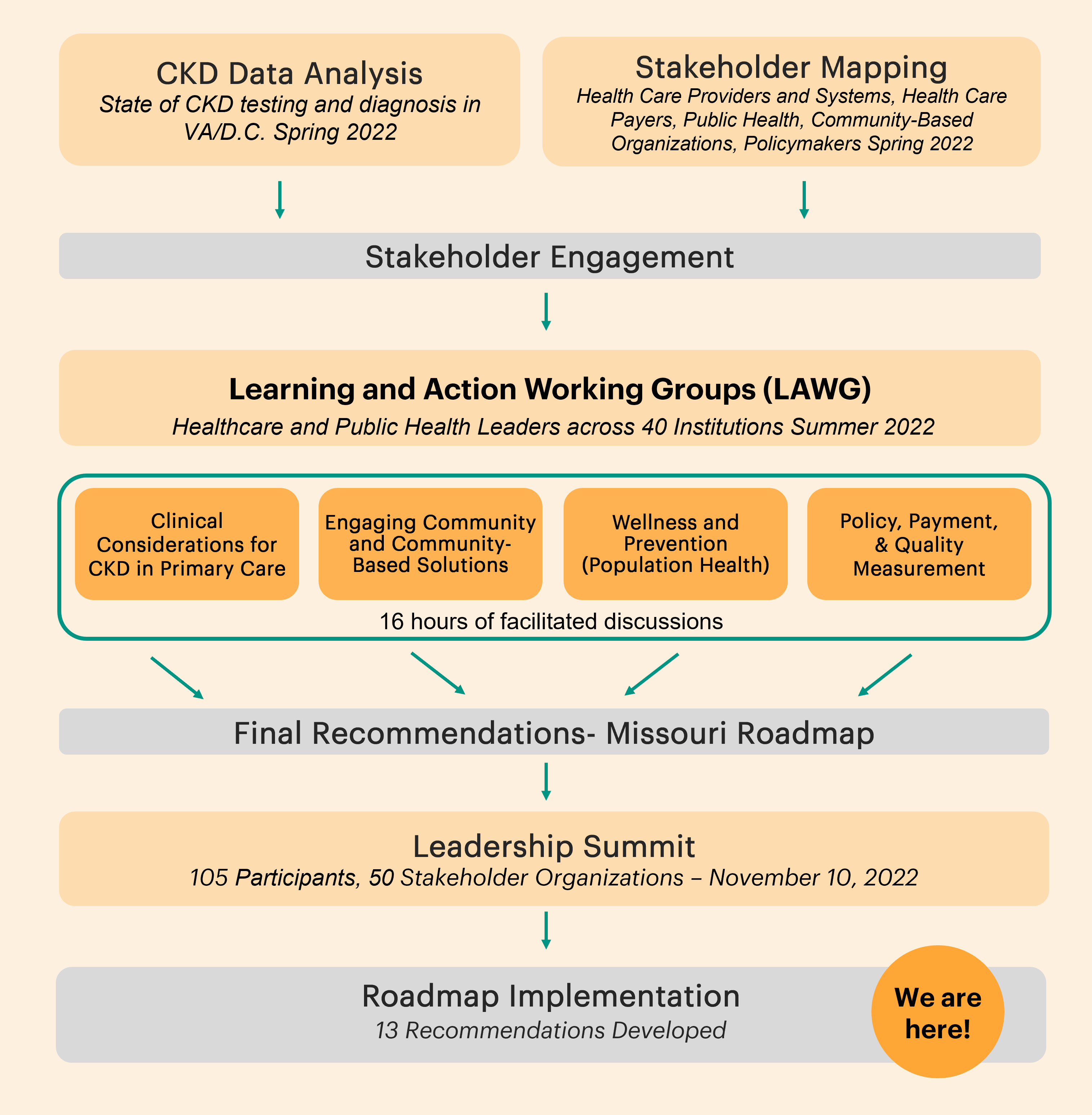
Learning and Action Workgroups
Through a series of facilitated discussions in Fall 2022, health care and public health leaders will identify barriers and solutions to improve CKD awareness, detection, and management in Virginia, and especially tools and strategies that can be implemented within stakeholders’ own institutions. The learning and action workgroups will support increased awareness and action amongst the participants. The four workgroups will convene covering the following topics:
Clinical Considerations for CKD in Primary Care
- Goal: To discuss strategies and approaches that can be employed to improve CKD recognition and care in primary care settings.
- Background: A large, national study illustrated that less than 12% of people with CKD were diagnosed in primary care.2 This included as many as 40% of people whose kidneys required specialty care. With the advent of new therapies demonstrated to slow or stop the progression of CKD, there is very real opportunity to improve quality of care for people with CKD across the entire spectrum of disease.
Engaging Community and Community- Based Solutions
- Goal: To develop strategies to advance CKD awareness through community engagement and to ensure that health care providers are aware of the community resources available to delay CKD progression.
- Background: In the US today, only 10% of people with laboratory evidence of CKD know that they have kidney disease.3 Improved patient awareness, engagement, and Self-Management are vital to successfully slowing CKD progression. As diabetes and hypertension play significant roles in the development of CKD, working with community organizations that support people with chronic disease can be an important step toward raising public awareness of CKD among those at risk for CKD.
Wellness and Prevention (CKD Population Health)
- Goal: To develop a strategy to incorporate CKD testing and diagnosis into wellness and prevention practices within the employer/commercial health plans, and the broader community.
- Background: To date, almost 90% of people living with CKD remain undiagnosed in the population and the majority will not receive guideline recommended annual testing.5 This breakout session will discuss the strategies that can be developed and employed to ensure that CKD testing and diagnosis are included as part of the wellness and prevention services, including corporate programs, diabetes prevention activities, etc., that are available in the state.
Policy, Payment, and Quality Measurement
- Goal: To develop a strategy to streamline CKD testing in primary care from a policy and payment perspective.
- Background: In July 2020, the NCQA released the Kidney Health Evaluation for Adults with Diabetes HEDIS measure (KHE).4 This measure assesses the percentage of people with diabetes that receive both tests for CKD during the course of a year. When tested against over 70 claims datasets, this measure was achieved in only 35% of cases. This measure will begin collecting data for public reporting in October 2021.
Roadmap
After multiple hours of facilitated discussion, 72 stakeholders identified strategies to improve testing, diagnosis and early management of CKD in Virginia. Read the roadmap summary here.
Leadership Summit
On November 10, 2022, NKF hosted a virtual summit to present recommendations and engage partners in joining the Collective Impact Approach. Over 150 registered and 105 attendees participated in this convening.
2022 Virginia Show Me CKD Intercept Stakeholders Conference Recording
Learn More and Join the Collective Impact Effort
Michele Anthony, MSA, Executive Director, National Kidney Serving the National Capital Area- michele.anthony@kidney.org
Nancy Castrina, Executive Director, The National Kidney Foundation of Virginia- nancy.castrina@kidney.org
Anna Fetzer, Population Health Partnership Director, anna.fetzer@kidney.org
References
- Hanley Brown, F. Kania, J. and Kramer, M. Channeling Change: Making Collective Impact Work. Stanford Social Innovation Review. 2012. https://doi.org/10.48558/2T4M-ZR69
- Szczech, Lynda A., et al. “Primary Care Detection of Chronic Kidney Disease in Adults with Type-2 Diabetes: The ADD-CKD Study (Awareness, Detection and Drug Therapy in Type 2 Diabetes and Chronic Kidney Disease).” Public Library of Science, 26 Nov. 2014. https://doi.org/10.1371/journal.pone.0110535
- “Chronic Kidney Disease (CKD) Surveillance System: Awareness.” Centers for Disease Control and Prevention. https://nccd.cdc.gov/ckd/detail.aspx?QNum=Q97#refreshPosition
- Brock, Matt. “Kidney Health: A New HEDIS Measure.” NCQA Blog, 16 Jul. 2020. https://blog.ncqa.org/kidneyhealth/
- “Chronic Kidney Disease in the United States, 2021.” Centers for Disease Control and Prevention, 4 Mar. 2021. https://www.cdc.gov/kidneydisease/pdf/Chronic-Kidney-Disease-in-the-US-2021-h.pdf