Last Updated: July 13, 2022
Medically reviewed by NKF Patient Education Team
About estimated glomerular rate (eGFR)
Your kidneys filter your blood by removing waste and extra water to make urine. The glomerular filtration rate (GFR) shows how well the kidneys are filtering. An estimated 37 million adults in the United States may have chronic kidney disease (CKD) but nearly 90% are unaware of their condition. When found early, people can take important steps to protect their kidneys.
Types
Measuring and estimating GFR
Getting an accurate GFR level is challenging because measured GFR (mGFR) is a complicated and lengthy process. This makes it impractical for both clinicians and patients. It is for this reason that healthcare professionals use a formula to estimate GFR. Often, CKD does not have any symptoms until the later stages of the disease. This is the reason why reliable estimates of GFR are so important for identifying CKD as early as possible.
The standard way to estimate GFR is with a simple blood test that measures your creatinine levels. Creatinine is a waste product that comes from the digestion of dietary protein and the normal breakdown of muscle tissue. Aside from CKD, creatinine levels can be affected by other factors including diet; muscle(weight of your muscles); malnutrition; and other chronic illnesses.
Differences between eGFR and mGFR
| Estimated GFR (eGFR) | Measured GFR (mGFR) | |
| How it works | A calculation used to estimate how well your kidneys are filtering certain agents produced by your body, such as:
| A measurement of how well your kidneys are filtering certain agents not produced by your body, such as:
|
| Availability | Widely available | Not widely available |
| Cost | Less expensive | More expensive |
| Time to complete the test | Less time needed | More time consuming |
| Accuracy | Possible inaccurate estimates of GFR, especially in early stages of kidney disease (stages 1 and 2)* | Accurate measures of GFR, including early stages of kidney disease (stages 1 and 2) |
| Precision | Can miss early GFR changes, such as a rapid decrease in levels, which may be a sign of diabetic kidney disease | Can identify early GFR changes, such as a rapid decrease in levels, which may be a sign of diabetic kidney disease |
*Other factors that can affect eGFR include: pregnancy, being over the age of 70, unusual muscle mass, cirrhosis (a disease caused by scarring in the liver), nephrotic syndrome (a condition caused by having too much protein in your urine), a past solid organ transplant, and some medications.
Purpose
Why eGFR testing is done
Early-stage CKD doesn’t usually cause symptoms, but your doctor may recommend an eGFR test if you are at higher risk of developing the disease. CKD risk factors include:
Diabetes
High blood pressure
Overweight/obesity
Over the age of 60
Family history of CKD or kidney failure
Usually, developing CKD is not due to any single reason, but because of a combination of physical, environmental, and social factors.
Later stage CKD does cause symptoms. So you may need an eGFR test if you have any of the following symptoms:
- Urinating more often or less often than usual
- Itching
- Feeling tired
- Swelling in your arms, legs, or feet
- Muscle cramps
- Nausea and vomiting
- Loss of appetite
One day, no one’s life will be lost to kidney disease.
- Equip patients and families with knowledge, resources, and access to high-quality care.
- Advocate for policies that address disparities and prioritize kidney health for all.
- Fund research and technology to advance early detection, improve treatment, and expand transplant access.
Results
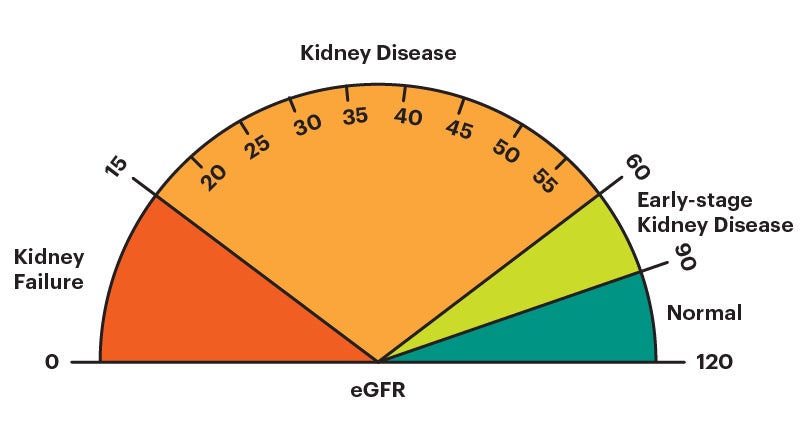
- eGFR of 90 or higher is in the normal range
- eGFR of 60 -89 may mean early-stage kidney disease
- eGFR of 15 -59 may mean kidney disease
- eGFR below 15 may mean kidney failure
What is a normal eGFR number?
In adults, the normal eGFR number is usually more than 90. eGFR declines with age, even in people without kidney disease. See chart below for average estimated eGFR based on age.
| Age (years) | Average eGFR |
| 20–29 | 116 |
| 30–39 | 107 |
| 40–49 | 99 |
| 50–59 | 93 |
| 60–69 | 85 |
| 70+ | 75 |
Understanding your results
There are five stages of kidney disease. Your healthcare professional determines your stage of kidney disease based on the amount of kidney damage shown by your eGFR or mGFR. Now that your know your eGFR, find out your kidney disease stage using the table below.
What are the stages of chronic kidney disease (CKD)?
| Stage | Description | eGFR | Kidney Function |
| 1 | Possible kidney damage (e.g., protein in the urine) with normal kidney function | 90 or above | |
| 2 | Kidney damage with mild loss of kidney function | 60-89 | |
| 3a | Mild to moderate loss of kidney function | 45-59 | |
| 3b | Moderate to severe loss of kidney function | 30-44 | |
| 4 | Severe loss of kidney function | 15-29 | |
| 5 | Kidney failure | Less than 15 |
What to do next
If you have any of the CKD risk factors listed above, ask your healthcare professional to order an eGFR lab test.
Questions for your healthcare team
Now that you know your eGFR and your stage of kidney disease, use this table to find questions to ask your healthcare professional at your appointments.
| If your kidney disease is in stage… | Ask your healthcare professional if you should… | |||||
| 1 | 2 | 3a | 3b | 4 | 5 | |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Test your urine for albumin to have a complete picture of your overall kidney health |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Repeat your eGFR test in 3 months to check if your eGFR remains lower than 90 |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Take medication that may help slow progression of kidney disease (such as ACE inhibitors, ARBs, SGLT2 inhibitors, or nonsteroidal mineralocorticoid receptor antagonists) |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Adjust any current medications due to reduced kidney function |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Get nutritional and dietary counseling to help support kidney function and overall health |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Start seeing a kidney specialist (nephrologist) |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Learn more about end-stage kidney disease and treatment options |
| ✔ | ✔ | ✔ | ✔ | ✔ | ✔ | Be evaluated for a kidney transplant and be placed on a kidney transplant list |
Kidney Numbers and the CKD Heat Map
Download a printable resource that explains what kidney numbers are and how your healthcare professional uses them to diagnose CKD.