August 12, 2014
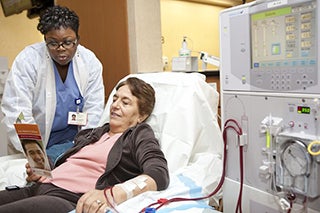 When you develop end stage kidney failure, your kidneys aren't able to function on their own anymore. This usually occurs when you lose about 85-90% of your kidney function. Dialysis can help those with kidney failure live longer, healthier lives, but as a patient, it may feel overwhelming to make decisions surrounding your treatment. It's important to realize that when it comes to your care, you have many rights and choices and the National Kidney Foundation encourages all patients to make informed decisions. Here are the National Kidney Foundation's Top 10 Things Every Dialysis Patient Should Know.
When you develop end stage kidney failure, your kidneys aren't able to function on their own anymore. This usually occurs when you lose about 85-90% of your kidney function. Dialysis can help those with kidney failure live longer, healthier lives, but as a patient, it may feel overwhelming to make decisions surrounding your treatment. It's important to realize that when it comes to your care, you have many rights and choices and the National Kidney Foundation encourages all patients to make informed decisions. Here are the National Kidney Foundation's Top 10 Things Every Dialysis Patient Should Know.
- You have treatment choices. Options exist for how, where and when you dialyze. Dialysis can be done in a hospital, in a dialysis unit that is not part of a hospital, or at home. You and your doctor will decide which place is best, based on your medical condition and your wishes. There are different types of dialysis - peritoneal and hemodialysis. Work with your health care team to determine a treatment plan that makes you feel comfortable. Recent studies show that the majority of patients beginning in-center hemodialysis (HD) know very little, if anything, about the option to dialyze at home. Once informed, 40% or more of patients are interested in this treatment option, and yet less than 10% actually begin home dialysis. If you're dissatisfied with the type of dialysis treatment that you're receiving, ask your healthcare team if another type of dialysis treatment would be better.
- You can compare in-center dialysis facilities online. Information on over 5,600 US-based dialysis centers is available online through the Medicare website. To help you make choices about your care, you can compare different facilities side-by-side and evaluate each facility based upon clinic characteristics and quality measures. You can search for dialysis facilities by name or geographic proximity. After completing an initial facility comparison to determine which facilities best meet your needs - such as the number of hemodialysis stations at a particular location and whether there are evening shifts available - visit the facilities that you're most interested in. Talk to the staff and other patients, as well as your doctor to ensure that this dialysis facility is a good fit for you.
- There are ways to prepare ahead for an emergency. Ask your dialysis facility about their emergency plan in case of a snow storm, fire, power outage or other natural disaster. As back up, make sure you have the names, locations and phone numbers of other dialysis units and hospitals in your area. Since regular community transportation services may not be working in an emergency, be prepared to make other arrangements for getting to dialysis. You may need to contact the police and Emergency Medical Services (EMS) for assistance. If you dialyze at home, make sure you have at least two weeks' worth of unexpired supplies on hand. If you have to miss a dialysis treatment, begin your emergency meal plan. Click here for more information about planning ahead for emergencies and to find a grocery list and meal plan for a 3 day emergency diet.
- There is an easy way to transfer patient records between clinics. There is an easy, secure way for your health care team to transfer your treatment records online. In 2009, the Centers for Medicare and Medicaid Services (CMS) created a centralized web-based data collection system called CROWNWeb to help reduce and eliminate patient treatment interruptions. This central system helps to streamline patient care regardless of the reason for changing dialysis centers. For example, if you've been admitted to the hospital, or if you needed to relocate during an emergency evacuation, your doctors and health care team can access up-to-date information about your dialysis so that you continue to receive appropriate care no matter where you are.
- You can travel while on dialysis. Dialysis centers are located in every part of the United States and in many foreign countries. The treatment is standardized, but you need to plan ahead by making an appointment for dialysis at another center before you go. The staff at your center may help you make these appointments.
- You can be your own best advocate. Know what key questions to ask your doctor or other healthcare professionals. Take notes so that you can refer back to them later. Partner with your doctor and decide on a treatment plan together. Advocate for yourself and share how you're feeling.
- You have many rights. You as a patient have a great deal of control over your treatments. Patients have a bill of rights which includes receiving quality care, counseling about your medical information, and an expectation of privacy. You also have responsibilities. Once you decide on a course of treatment, it's important to follow the recommendations of your health care team. If you decide to receive in-center dialysis, arrive at dialysis on time so that you can receive the full treatment without delays.
- You can receive insurance coverage. If you have end stage renal failure, you are likely eligible for Medicare insurance coverage. Speak with your health care team and social worker for help filling out insurance paperwork.
- You may need to follow a special diet. When your kidneys are not working properly, you may not be able to eat everything you like, and you may need to limit how much you drink. Your diet may vary according to the type of dialysis you receive. It is important to speak with a renal dietitian so that you are able to understand what you can and cannot eat based on your full health history.
- Dialysis patients can work. Many dialysis patients can go back to work or school after they have gotten used to dialysis. After establishing a dialysis routine, many patients have more energy and find that they are able to time to work around this new schedule. Some patients even find creative ways to work remotely from dialysis with the use of a laptop or cell phone, depending on their field of expertise.