Last Updated: January 02, 2023
Medically reviewed by NKF Patient Education Team
About Dialysis
Dialysis is a type of treatment that helps your body remove extra fluid and waste products from your blood when the kidneys are not able to. Dialysis was first used successfully in the 1940's and became a standard treatment for kidney failure starting in the 1970s. Since then, millions of patients have been helped by these treatments.
Dialysis can be done in a hospital, a dialysis center, or at home. You and your doctor will decide which type of dialysis and which place is best, based on your medical condition and your wishes.
Uses
Dialysis is helpful for two different situations:
- Acute kidney injury (AKI): a sudden episode of kidney failure or kidney damage that happens within a few hours or days. AKI is usually treated in a hospital setting with intravenous fluids (given through the vein). In severe cases, dialysis may also be needed for a short time until the kidneys get better.
- Kidney failure: when 10-15% of your kidney function remains, measured by an estimated glomerular filtration rate (eGFR) of less than 15 mL/min. At this stage, your kidneys are no longer able to keep you alive without some extra help. This is also known as end-stage kidney disease (ESKD). With kidney failure, dialysis is only able to do some of the work of healthy kidneys, but it is not a cure for kidney disease. With ESKD, you will need dialysis for the rest of your life or until you are able to get a kidney transplant.
How it works
Dialysis performs some of the duties that your kidney usually does to keep your body in balance, such as:
- removing waste and extra fluids in your body to prevent them from building up in the body
- keeping safe levels of minerals in your blood, such as potassium, sodium, calcium, and bicarbonate
- helping to regulate your blood pressure
Types
Hemodialysis (HD)
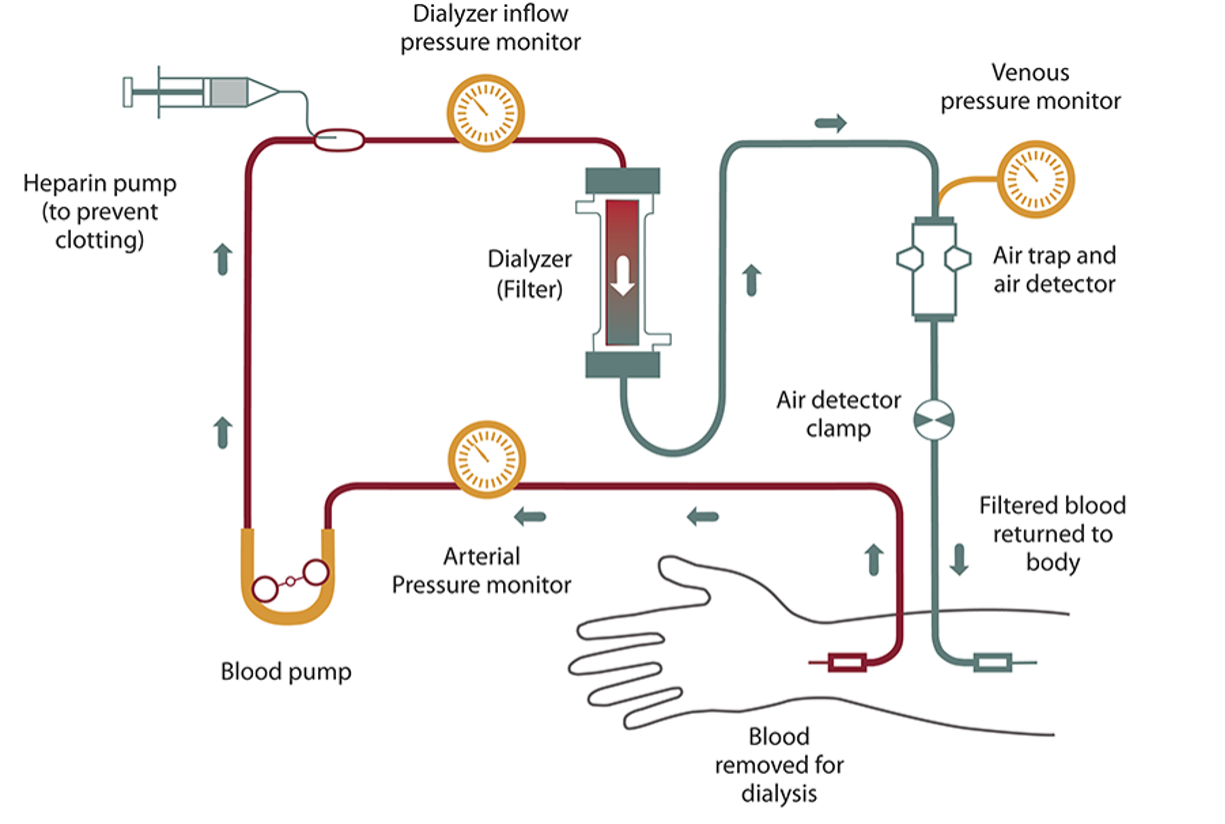
In hemodialysis, a dialyzer (filtering machine) is used to remove waste and extra fluid from your blood, and then return the filtered blood into your body. Before starting hemodialysis, a minor surgery is needed to create a vascular access site (opening into one of your blood vessels), usually in your arm. This access site is important to have an easy way to get blood from your body, through the dialyzer, and back into your body. Hemodialysis can be done at a dialysis center or at home. Treatments usually last about four hours and are done three times per week. Some people may need more time for treatments based on their specific needs.
Peritoneal Dialysis (PD)
In peritoneal dialysis, your blood is filtered inside your own body instead of using a dialyzer machine. For this type of dialysis, the lining of your abdomen or belly area (also called the peritoneum) is used as a filter. Before starting peritoneal dialysis, a minor surgery is needed to place a catheter (soft tube) in your belly. During each treatment, your belly area is slowly filled with dialysate (a cleansing fluid made from a mixture of water, salt, and other additives) through the catheter. As your blood flows naturally through the area, extra fluid and waste products are pulled out of the blood vessels and into the belly area by the dialysate (almost like a magnet). After a few hours, the fluid mixture is drained from your belly using the same catheter and bag that was used at the beginning of the treatment. Peritoneal dialysis can be done almost anywhere if you have the supplies required to perform the treatment.
Two of the most common types of peritoneal dialysis are:
- Continuous Ambulatory Peritoneal Dialysis (CAPD)
- Automated Peritoneal Dialysis (APD)
The supplies and equipment needed, duration of each treatment (also known as an exchange), and number of treatments per day will differ depending on the type of PD you are using and your medical condition. More information about these treatments can be found on the NKF Peritoneal Dialysis AtoZ page. 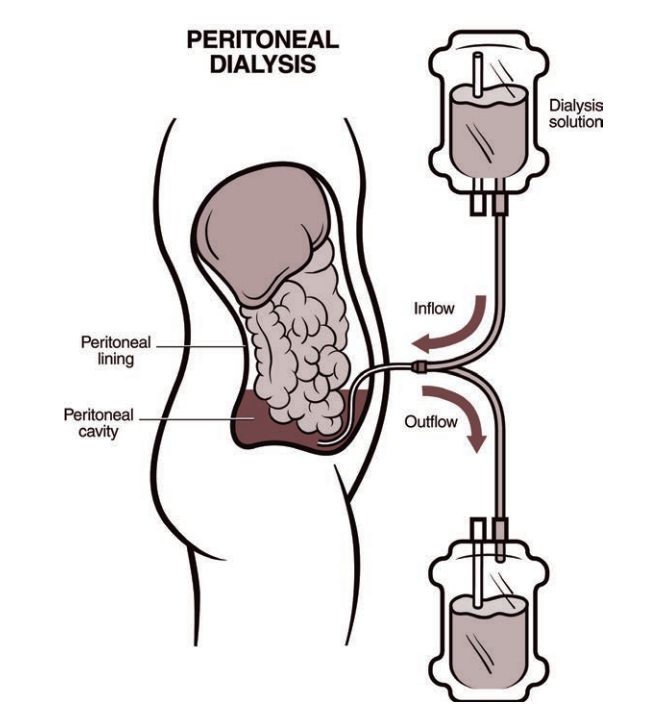
One day, no one’s life will be lost to kidney disease.
- Equip patients and families with knowledge, resources, and access to high-quality care.
- Advocate for policies that address disparities and prioritize kidney health for all.
- Fund research and technology to advance early detection, improve treatment, and expand transplant access.
Effectiveness
Dialysis is a very effective treatment option for clearing waste products and extra fluid from your blood. However, it does not fully replace all the kidney’s functions, so it is not considered a cure for kidney disease or kidney failure.
All types of dialysis are equally effective, but your medical condition and personal preferences may match one treatment approach better than others. You and your doctor will discuss this and decide which type of dialysis and which place is best. You may also find it helpful to talk with other people who are living with dialysis to learn from their experiences.
The following steps can help increase the effectiveness of your dialysis treatments:
- complete your treatments according to your prescribed schedule
- follow your customized eating plan recommended by your kidney dietitian
- get as much physical activity as possible to boost your strength and heart health
- talk with your dialysis provider and pharmacist about any medications, supplements, or herbal products you are taking or are considering starting
- talk with your dialysis team about any concerns or side effects that you may have
Every person responds differently to dialysis, and your level of risk for each side effect will differ from others. If you have concerns about any of these risks, talk to your doctor and dialysis team about ways you can lower your risk. Although these side effects may sound scary, they should be compared to the risks that come from continuing to live with untreated kidney failure.
Additional Considerations
Impact on regular routine
Most people on dialysis are able to keep a regular routine except for the time needed for treatments. Dialysis often makes people feel better because it helps clear the waste products that have built up in the blood between treatments. However, some people report feeling tired after dialysis, especially if they have been getting dialysis treatments for a long time.
People receiving dialysis treatments also need to be mindful of what they eat. The specific meal plan recommended for you may vary depending on which type of dialysis you receive. Work with your kidney dietitian to create a meal plan that fits your routine and lifestyle.
Traveling is also a possibility for people on dialysis. Dialysis centers are in every part of the United States and many other countries. The treatment is standardized. You must make an appointment for dialysis treatments at another dialysis center before you go. The staff at your current center may help you make the appointment. Visit the NKF Travel Tips AtoZ page for more information.
Many people on dialysis can go back to work after they have gotten used to dialysis. However, if your job has a lot of physical labor (heavy lifting, digging, etc.), you may need to look for a different type of work. Visit the NKF Working with Kidney Disease AtoZ page for more information.
It will likely take you and your family some time to get used to including dialysis treatments into a new routine.
Costs
Dialysis treatments are very expensive. However, most people with kidney failure are eligible for Medicare when they start dialysis. This means the federal government pays 80 percent of all dialysis costs. Private health insurance or state Medicaid programs may also help with the costs. Visit the NKF resource on insurance options for people on dialysis or with a kidney transplant to learn more.
Discomfort
You may have some discomfort as the needles are put into your access site. Over time, people usually get used to being around these needles and equipment. The dialysis treatment itself is painless.
Life Expectancy
Life expectancy on dialysis varies depending on your other medical conditions, how well you follow your treatment plan, and various other factors. The average life expectancy on dialysis is 5-10 years. However, many patients have lived well on dialysis for 20 or even 30 years. Talk to your healthcare team about how to take care of yourself and stay healthy on dialysis.
Preparing for Your Appointment
Questions to Ask
- Which type of dialysis might work best for my situation?
- Would I be a candidate for completing my dialysis treatments at home?
- How do I determine which dialysis center I should go to?
- How can I lower my risk of infection and other side effects while on dialysis?
- Do I need to adjust any of my medications because of these dialysis treatments?
- What type of meal plan should I be following while I’m on dialysis?
- How can I get added to the kidney transplant waitlist?
Dialysis
Sign up for a deep dive into dialysis
Learn about the different types of dialysis, receive additional resources, and learn so much more.









