
Overview
The goal of the NKF Ending Disparities in CKD Leadership Summit is to drive a cultural shift in primary care toward increasing the early diagnosis and management of chronic kidney disease (CKD) in Greater Philadelphia. Using the Collective Impact model as a framework, NKF convened stakeholders from across health care delivery, payers, public health, and the community to develop and advance equitable strategies to improve CKD testing and diagnosis in primary care across the region.
Through a series of Learning and Action Workgroup discussions stakeholders identified barriers and solutions to improve CKD awareness, detection, and management in Greater Philadelphia. In total, 42 stakeholders representing 27 organizations across the region participated in these workgroup discussions.
On June 11, 2025, NKF hosted a summit at Thomas Jefferson University Hospital to present the final recommendations and engage partners in joining the Collective Impact approach. Eighty-nine individuals registered and 70 attended the live Summit with 81 commitments made to support implementation of the 12 recommendations.
Methods
NKF convened health care, public health, and community stakeholders from across the Greater Philadelphia Area to participate in workgroups that focused on Clinical Considerations for CKD in Primary Care, Engaging Community and Community-Based Solutions, Policy, Payment, and Quality Measurement, and Wellness and Prevention in CKD. During these meetings, participants:
- Analyzed the prevalence of undiagnosed chronic kidney disease (CKD) in Greater Philadelphia, and its impact on patient outcomes, healthcare costs, and health inequities.
- Discussed strategies and approaches that can be employed to improve CKD recognition and care in primary care settings.
- Evaluated the impact the Kidney Health Evaluation HEDIS and MIPS measures can have on improving breakdowns in care and developed a strategy to streamline CKD testing in primary care from a policy and payment perspective.
- Developed a strategy to incorporate CKD testing and diagnosis into population health, community wellness and prevention practices.
- Developed strategies to advance CKD awareness through community engagement and to ensure that health care providers are aware of the community resources available to delay CKD progression.
Results of the Discussions
Barriers to improved CKD testing and diagnosis
Knowledge, perceptions, and ongoing training among primary care clinicians are areas needing significant improvement. There are knowledge and perception gaps present surrounding the CKD screening guidelines, the impact of CKD on cardiovascular health, and how to effectively manage CKD in primary care with medications. Additionally, many primary care providers lack the necessary knowledge and training to prioritize CKD, leading to late diagnoses and inadequate patient education on disease management. It is critical to not only close these gaps but also to see that confidence in managing CKD in primary care translates to action in patient care.
Health system infrastructure and workflow barriers also hinder CKD management. Clinical workflows, operations, and electronic health record (EHR) tools are not always optimized for CKD identification and management, creating inefficiencies and barriers to care. There is a need for more tools and resources to help care teams efficiently diagnose, test, and manage CKD through effective communication and documentation. Establishing effective communication and referral pathways between healthcare and community-based resources or programs is crucial to prevent delays and confusion in patient care. Additionally, initiating some knowledge sharing between organizations with the same goals, to reduce costs and improve patient care and outcomes, can help to drive improvements regionally.
Insufficient quality measures and limited payer prioritization result in inadequate support for CKD screening and management. Reimbursements and funding don’t currently support prioritizing CKD directly as there is limited recognition on the impact/relevance of CKD on other quality goals among payers. Additionally, there is limited awareness of the impact of CKD on costs, quality rates, etc. which leads to few or no payment models that emphasize CKD. And for members, there is a lack of incentives for CKD among health plans.
Access to primary care and social determinants of health provide significant barriers for individuals, especially as visits with labs or additional testing often needing a separate appointment at a separate location. This provides challenges for patients with limited time off, difficulty with transportation, or other social determinates of health factors that make access difficult. Many patients are unaware of the risk factors contributing to CKD and the available prevention and management programs. Chronic disease self-management programs are underutilized, and there is a general lack of urgency in managing CKD, both from the patients’ and providers’ perspectives.
Lastly, public perceptions and awareness about CKD are critically lacking among both the public and healthcare providers. Patients often do not understand the implications of CKD, leading to a sense of resignation and a lack of proactive management. Many people have competing priorities and must make decisions based on limited time and resources, as early CKD is asymptomatic, it is often not considered a priority. Public education campaigns need to be more effective, targeting appropriate literacy levels and using diverse media channels. There is also a pervasive misconception that CKD is untreatable, which hampers efforts to increase patient activation and self-care.
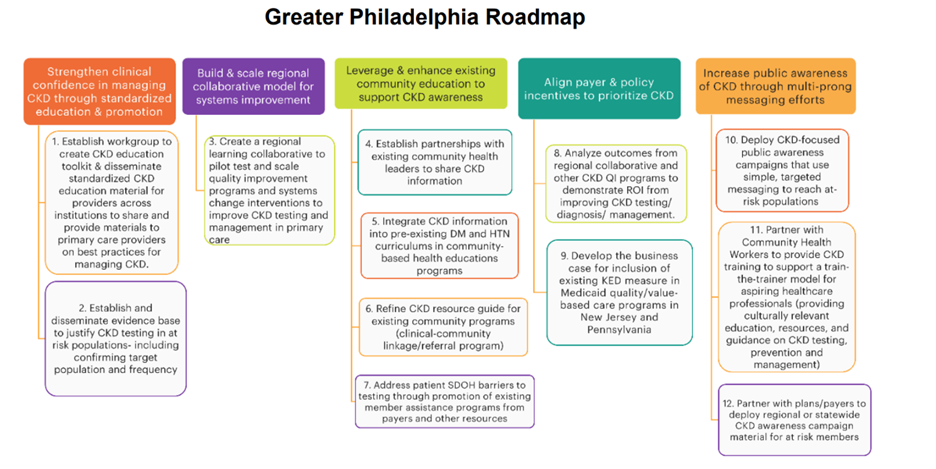
Summit Data and Recommendations
- Strengthen clinical confidence in managing CKD and understanding of the importance through standardized education and promotion of evidence-based guidelines.
- Establish a workgroup to create CKD education toolkit & disseminate standardized CKD education material for providers across institutions to share, including best practices for managing CKD in primary care.
- Establish & disseminate evidence-base to justify CKD testing in at-risk populations – including confirming target population & frequency.
- Build & scale regional collaborative models for systems improvement to improve CKD testing and management outcomes.
- Create a regional learning collaborative to pilot test and scale quality improvement programs and systems change interventions to improve CKD testing and management in primary care.
- Align payer & policy incentives to prioritize CKD.
- Demonstrate ROI from improving CKD testing/diagnosis/management
- Develop the business case for inclusion of existing KED measure in Medicaid quality/value-based care programs in New Jersey & Pennsylvania
- Leverage and enhance existing community outreach and health education resources to support CKD-based awareness and education
- Establish partnerships with existing community health leaders to share CKD information.
- Integrate CKD information into pre-existing diabetes and hypertension curriculums in community-based health education programs.
- Refine CKD resource guide for existing community programs (clinical-community linkage/referral program).
- Address patient social determinants of health (SDOH) barriers to testing through promotion of existing member assistance programs from payers and other resources.
- Increase public awareness of CKD through multi-prong messaging efforts.
- Deploy CKD-focused public awareness campaigns that use simple, targeted messaging to reach at-risk populations.
- Partner with community health workers (CHW) to provide CKD training to support a train-the-trainer model for aspiring healthcare professionals.
- Partner with plans/payers to deploy regional or statewide CKD awareness campaign material for at-risk members.
Previous Event Details
Wed, 06/11/2025 - 08:00am to 12:00pm
Thomas Jefferson Alumni Hall- Phone: 215.923.8611